Summer is here and families everywhere are planning outdoor adventures after nearly two years of social isolation. Calendars are now packed with camping trips, bonfires, hikes, and days on the lake. The summer of 2021 is well-deserved, and your friends at Madsen Pest Management have some tips to share as you venture outdoors to keep you and your loved ones safe.
Whether it’s hunting, fishing, or conquering wooded trails, you are bound to encounter wildlife. While the creatures you encounter may seem innocent and even cute, some animals can be dangerous and have the potential to spread infectious diseases. In this blog, we will discuss some of those diseases, the animals that carry them, the tell-tale symptoms of infection, and share some information that will help you stay protected.
PLAGUE
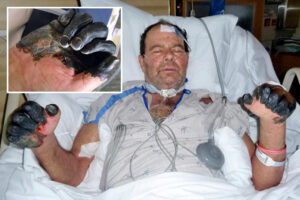
Don’t worry – we won’t be seeing a full-force comeback of the “Black Death” plague that ravaged Europe in the Middle Ages. But believe it or not, The Plague (while not widespread) still does exist right here in the United States.
For those of you in our service range (Northwestern Wisconsin and Northeastern Minnesota), you can breathe a little easier as most of the animals with the highest rate of plague cases are found in the Southwestern parts of the US. This infection is typically carried by the fleas found on rats, ground squirrels, rabbits, prairie dogs and ferrets.
There are two types of plague that can be found in humans (bubonic and pneumonic). The bubonic form is characterized by a bacterium and infected lymph nodes. The pneumonic form is characterized by acute pneumonia and is much more contagious and rapidly fatal if untreated (Statistics show a 100 percent mortality within one to three days).
Immunization is the most common way to protect yourself from the plague. When it comes to pests, you will want to steer clear of dead animal carcasses. Fleas can also spread the plague to humans. Use PPE (Personal Protective Equipment) if you are an avid hunter and handle dead animal carcasses.
Since tracking has begun, there has never been a reported case of plague in Wisconsin or Minnesota.
RABIES
 A commonly known infectious disease, rabies is regularly related to pests. Many rabies cases occur in wild animals like raccoons, skunks, bats, and foxes. These pests can transmit rabies to humans via bites or any other situation where the pest’s saliva gets into an open wound. Although less common, rabies can be spread by breathing in an area where infected animals reside. This makes bat caves and even un-managed bat infestations dangerous if left unattended.
A commonly known infectious disease, rabies is regularly related to pests. Many rabies cases occur in wild animals like raccoons, skunks, bats, and foxes. These pests can transmit rabies to humans via bites or any other situation where the pest’s saliva gets into an open wound. Although less common, rabies can be spread by breathing in an area where infected animals reside. This makes bat caves and even un-managed bat infestations dangerous if left unattended.
Rabies infects the central nervous system and the brain, ultimately causing death. Early symptoms of rabies include fever, headache, and general weakness or discomfort. As the disease progresses, more symptoms appear such as anxiety, confusion, paralysis, agitation, hallucinations, hypersalivation (increase in saliva), difficulty swallowing, and hydrophobia (fear of water). Death usually occurs within days of the onset of these symptoms and once rabies has developed, there is no clear path to treatment. Thus, early preventive measures remain the only way to guarantee survival after a bite by a rabid animal.
Immunization and contact avoidance are the two best ways to prevent contracting this fatal infection. People who encounter wildlife should be vaccinated against rabies. Otherwise, the best protection for people and their pets is to avoid being bitten. In case of a bite from a wild mammal, it is important to seek immediate medical care because rapid treatment with rabies immunoglobulin (antibodies) and vaccination can sometimes block the infection before it becomes fatal.
HANTAVIRUS
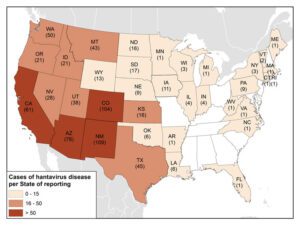
Courtesy of cdc.gov
Unlike the plague or rabies, which have been well recognized for centuries, Hantavirus has only recently become recognized.
In the United States, deer mice are a common transmitter of the virus. These rodents can spread the virus in their urine, droppings, and saliva. The infection can be transmitted to people when they breathe air contaminated by airborne particles of fresh rodent urine, droppings, or nesting materials. Additionally, Hantavirus can be transmitted through bites from infected mice, although this transmission is less common.
Early-onset of Hantavirus infection includes flu-like symptoms such as fever, cough, muscle aches, headache, and fatigue. However, the life-threatening form of infection, Hantavirus Pulmonary Syndrome, is characterized by a sudden onset of shortness of breath with rapidly evolving pulmonary distress that can be fatal in half the cases.
Anyone who encounters rodents that carry Hantavirus is at risk for infection. Rodent infestations can put people at risk for Hantavirus exposure and can occur in and around your home, and in structures like cabins, barns, or campgrounds.
Prevention and control are the primary strategies for avoiding contact with infected rodents. People who live in areas where Hantavirus is common (only 5 reported cases in Wisconsin since 2000) should contact a licensed pest professional to outline the best prevention plan and elimination techniques in case of an infestation.
TULAREMIA
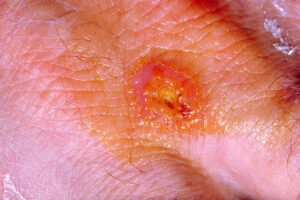
Courtesy of wikipedia.org
Humans can become infected with Tularemia through contact with infected animals or carcasses, or from a bite by infected ticks, deer flies, and other insects. Transmission is also possible through the inhalation of airborne bacteria and ingestion of infected food or water. In the summer, most cases come from infected tick bites. In the winter, cases are reported by hunters who trap and skin infected animals. Person-to-person transmission of Tularemia does not occur.
Inhalation of the bacteria leads to Pneumonic Tularemia, the most severe form of the disease. Pneumonic Tularemia is characterized by non-specific respiratory symptoms including hemorrhagic inflammation of the lungs and bronchopneumonia. This, in addition to low suspicion of Tularemia (due to its relatively low occurrence), makes it challenging for physicians to correctly diagnose isolated cases.
The symptoms of Tularemia infection may range from asymptomatic illness to septic shock and death, depending on the virulence of the infecting strain, portal of entry, inoculums (number of bacteria a person is exposed to) and the immune status of the host. Another common type of Tularemia is Ulceroglandular Tularemia, which normally results from the bite of infected ticks, or contact between broken skin and direct contact with the virus.
Symptoms can appear abruptly (three to five days after infection) but can take as long as two to three weeks to appear. Fever is the most common symptom of Tularemia, and others include joint pain, chills, loss of appetite, malaise, swollen lymph nodes, headache, chills, dry cough, sore throat and ulcers at the site of infection, sore eyes, weakness and diarrhea.
Immediate treatment with the appropriate antibiotics is recommended, as Tularemia can be fatal if left untreated. Tularemia is found across the United States, but Wisconsin only averages one case per year since 1980.
Diagnosis is made on a combination of suspicious signs and symptoms, followed by laboratory confirmatory testing. Treatment typically requires intramuscular or intravenous antibiotic therapy for 10 days.
Although these wildlife diseases are dangerous and pose a significant risk to humans, they are not a reason to stop enjoying the great outdoors. By following a few simple precautions, humans can safely interact with wildlife and keep any health dangers at bay. Contact Madsen Pest Management for more information or to report pest infestations and activity.
RELATED POSTS

Rodents in My House? How To Perform Your Own Inspection
madsen0319
•
February 24, 2021
•
Do It Yourself Pest Management, Home Pest Management Tips, House Protection, Rodents Prevention and Maintenance
•
No Comments
This blog will teach you how to inspect your home for rodent activity.

Mouse Math – How Fast Do Mice Multiply?
madsen0319
•
February 23, 2021
•
Rodents Prevention and Maintenance
•
No Comments
To some, mice might seem harmless, maybe even cute. But these little critters can wreak havoc on your home or business. A …

Rodent Problems and Infestations: How to Determine Severity
madsen0319
•
February 23, 2021
•
Rodents Prevention and Maintenance
•
No Comments
Addressing a rodent problem typically comes on the heels of watching one suddenly scamper across the floor at home. Fortunately, there are …
Related Posts
Pest Infestations During Mild or Late Cold Weather Seasons
Late starts to Fall and Winter with increasingly moderate temperatures are now common in Wisconsin and Minnesota. Due to this reality, prolonged pest activity may occur in and around your property.
Signs of Wasp Infestation and Preventative Measures
Wasps are one of the more aggressive stinging insects you can encounter. While many species of bees only sting once, wasps can sting multiple times. Their stings can be painful and if you are allergic, they can also be dangerous.
Flies and Food Contamination
Flies carry some dangerous diseases and parasites including gangrene, dysentery, tuberculosis, anthrax, and even the plague!



